By Katie E. Golden, MD
By Katie E. Golden, MD
We are amidst another surge in COVID cases, and it feels like there are new variants and scientific studies debuting every day. The treatment options are no exception. While we know a lot more about the coronavirus than we did a year ago, the growing list of possible treatments still remains in the early experimental phases.
If you have recently been diagnosed with COVID, you may be wondering what you can do to recover as quickly as possible. Or maybe you are worried about your infection getting worse. With so much information out there, It can be hard to figure out the best way to take care of yourself or a loved one. But before you tune into the chatter about different treatments — antibodies, ivermectin, azithromycin — let’s take a look at what the scientific evidence tells us about these medications.
This article is intended to provide you with a review of the treatments that are currently dominating the conversation for outpatient (non-hospitalized) people. And what to do if you have more questions about them.
What COVID-19 treatments are currently available?
It’s hard to keep track of all of the proposed treatment options for COVID-19. There is medicine traditionally used for malaria or autoimmune disease . . . blood transfusions from people who recovered from the infection . . . and what about that horse medicine for worms? So before we address the outpatient options, let’s review the broad picture of the COVID-19 treatment landscape.
It helps to think of COVID treatments in three general categories:
- Antiviral treatments inhibit the virus’s ability to replicate inside the human body. There are many of them out there, but the main ones include:
-
- Remdesivir. This is the only FDA-approved medicine for COVID, and it is only being used for people who are hospitalized with severe and life-threatening cases.
- Ivermectin. This medicine has been around for a long time, but it has recently received a lot of attention. It is used to treat rare worm and parasite infections, but has never been used to treat viruses, and there is no current evidence supporting its use in COVID. What’s worse, people are getting sick when they take it, especially in doses intended for animals and not humans. Experts are issuing serious warnings NOT to take this medication. There’s a good reason ‘horse pills’ don’t go down easy.
- Azithromycin. This is a well known antibiotic that is used to treat respiratory and lung infections caused by bacteria. There is no evidence that supports its use in a COVID infection. It gained traction as a possible treatment when one research study combined it with hydroxychloroquine (discussed below) to treat COVID patients, but this study did not have a control group and the results were not informative. Health institutes, like the NIH, do not recommend its use for COVID.
- Anti-inflammatory treatments dampen the immune system’s response to pathogens or proteins that stimulate the immune system. This may seem like a counterintuitive approach to fighting an infection, however some of the complications that develop from COVID are actually damage from the inflammation generated by the immune response, rather than the virus itself.
- Hydroxychloroquine (chloroquine, Plaquenil) is a medication used to treat malaria, as well as autoimmune diseases like rheumatoid arthritis or lupus. It has a complicated way of working in the body, and is actually sort of a hybrid antiviral and anti-inflammatory medication. Despite its theoretical potential in helping COVID patients, it has not proven to be beneficial in numerous research studies. In fact, one of these clinical trials was stopped early given its lack of benefit and potential harm. And in another study, initial data actually showed that it increased the risk of a patient requiring a ventilator. So unless you take this medication for a different medical condition, it is potentially dangerous and not recommended.
- Steroids (dexamethasone, decadron, solumedrol, prednisone) have had an on-again, off-again relationship with COVID. In other words, it’s complicated. Current evidence suggests that steroids may be beneficial for people with more severe cases (like hospitalized patients who are requiring oxygen). They have not seen any benefit in people with COVID who are not in the hospital, so like Remdesivir, this is only recommended as treatment for hospitalized patients.
- Antibody treatments are designed to provide someone with virus-fighting antibodies while their own immune system works to ramp up production. This is particularly helpful for people who may have trouble mounting a strong immune response to a COVID infection, like those with a weaker immune system.
- Monoclonal Antibodies have some promise as a potential treatment for people with weaker immune systems. They are similar to the antibodies our immune system makes when exposed to the virus (or the vaccine), but they are made in a factory instead. Given this treatment may be beneficial, we will go over it in further detail below.
- Convalescent Plasma comes from the blood of people who have recovered from COVID. The theory is that this provides antibody-rich blood that will help fight the virus for those who are actively infected. While this is being investigated, there is no current evidence that shows it is beneficial, and thus the NIH does not recommend it be used until we can collect more data.
What COVID-19 treatments are currently recommended?
Now that you have the lay of the land of COVID treatments, let’s provide a key point summary:
- Remdesivir and steroids have shown some benefit in people with severe cases, so these treatments are being used in hospitalized patients.
- For people who do not need to be in the hospital, monoclonal antibodies may help people who are at risk for more severe disease because of a weaker immune system.
- Ivermectin, hydrochloroquine, azithromycin, gargling with industrial antiseptic solutions, and injecting oneself with bleach are not recommended. And may be harmful.
Do I Need Monoclonal Antibodies?
Monoclonal Antibodies (MABs) are designed to provide antibodies (virus-fighting proteins) to people when their own immune system can’t make enough of them, or can’t make them very quickly. This may be true for people who have medical conditions that weaken their immune system. The goal of this treatment is not necessarily to cure the infection or decrease the duration of illness, but rather to prevent their infection from getting worse to the point that they would require hospitalization.
There are several different types of monoclonal antibodies, each of them with their own difficult-to-pronounce names (bamlanivimab, etesevimab, casirivimab, imdevimab, sotrovimab, whenwillthispandemicbeovermab . . . okay that last one I just made up).
There have been numerous research studies investigating different MABs, or combinations of MABs, and the results are mixed. This is partially attributed to the likelihood that some MABs are more effective than others in fighting evolving variants. But here’s a general summary:
- In some randomized, placebo-controlled trials (read: high quality study designs), outpatients with increased risk for severe disease had reduced risk of both hospitalization and death.
- These potential benefits have not been seen in hospitalized patients, and one study was even stopped early when it was obvious the treatment was not helpful.
- Laboratory studies (we’re talking petri dishes and not real humans) suggest that newer variants may render certain MAB treatments less effective.
There are a lot of smart people at well respected institutions (like the NIH, CDC, and FDA) who disagree on which MABs should be authorized for emergency use. And this is because there simply isn’t enough data to make a unified decision. But the good news is that researchers are working hard to provide some answers,
In the meantime, these experimental treatments are available for certain patients based on preliminary data. So who gets them? Here are the current guidelines:
- MABs are available for non-hospitalized patients with COVID-19 who are at high risk of severe disease, as long as they are within 10 days of symptom onset (given the treatments are unlikely to be helpful beyond this time point).
- Patients that saw a benefit with treatment in clinical trials had the following risk factors:
- Age 65 years or older
- Body size that correlates to a BMI > 30
- Diabetes
- Cardiovascular disease (like coronary artery disease and hypertension)
- Chronic lung diseases (like COPD, moderate or severe asthma, interstitial lung disease, cystic fibrosis, pulmonary hypertension)
- While the above risk factors were formally studied, the CDC has also extended this treatment option to people with other conditions that may put them at higher risk for severe infection:
- An underlying immunocompromised condition, or immunosuppressive medication
- Body size that correlates to a BMI of 25–30
- Chronic kidney disease
- Pregnancy
- Sickle cell disease
- Neurodevelopmental disorders (such as cerebral palsy)
- Dependence on medical devices, such as ventilation through a tracheostomy, gastrostomy (a feeding tube), or positive pressure ventilation (severe obstructive sleep apnea that requires a CPAP machine)
How do I get monoclonal antibody treatment?
If you have COVID and qualify for antibody treatment, the first step is to discuss the risks and benefits of treatment with a trusted provider. This conversation is most helpful with a healthcare professional who knows you and your medical history well, as they will have the best insight into your unique case and risk factors. But of course, any primary care provider is equipped to answer your questions and help you figure out if MAB treatment is right for you.
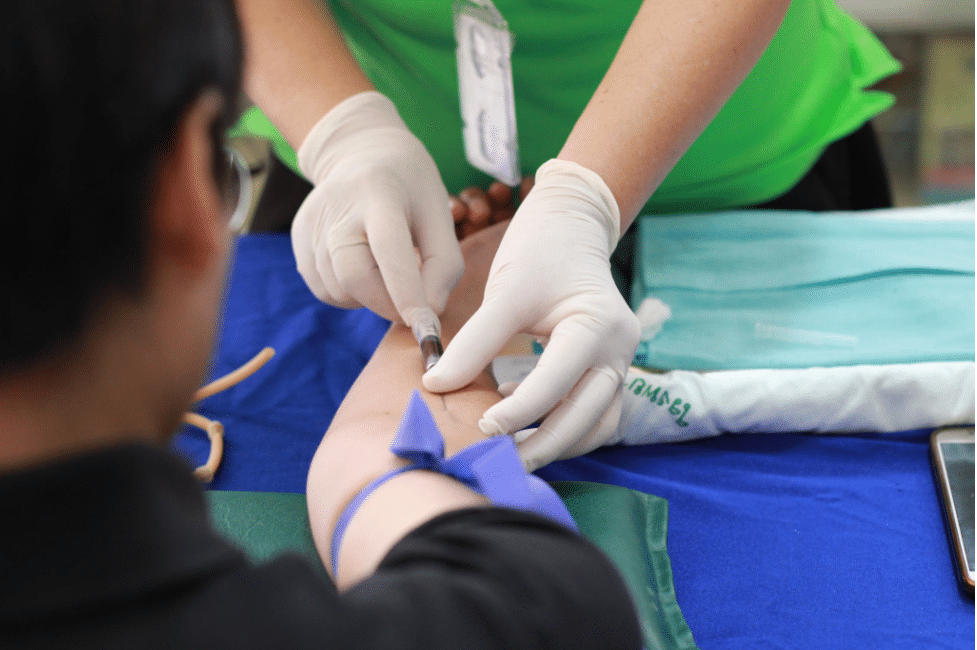
MAB treatments are administered as an infusion, which means it is administered through an intravenous (IV) catheter and goes straight into your veins. Most hospital systems have equipped their outpatient infusion centers to deliver these medications. These are clinics that also specialize in providing treatments like blood transfusions and chemotherapy infusions. The providers who work there are best suited to administer MABs given their familiarity with treatment and dosing protocols, as well as their ability to monitor and recognize adverse reactions to the medication. Your primary care provider can help connect you with an infusion center that specializes in MAB treatment.
In conclusion, remember that it can be tempting to seek out experimental treatments for COVID when you or a loved one is diagnosed with the infection. But it’s important to take a step back, and understand the research on these treatments, as well as the risks of receiving a medication that can be potentially harmful. Rest assured that some of the best medicine is produced by your own body, and with rest and support (and maybe a Netflix marathon), it will provide a full recovery.