By Katie E. Golden, MD
By Katie E. Golden, MD
Parents often bring their children into the Emergency Department (ED) for evaluation of fever, which is a common occurrence in babies, infants, and toddlers.
Their young immune systems are still learning how to build a defense system against all those viruses and bacteria that surround them on a daily basis, to which they are frequently exposed: doting grandparents who shower them with kisses, dog bones that double as teething toys when mom is not looking, and daycare centers with a germ load equivalent to the monkey house from The Hot Zone. And every parent knows that trying to get a 2 year old to practice good hand hygiene can be as impossible as asking them to eat broccoli for breakfast. For all these reasons and more, kids tend to spike fevers more frequently (and to higher temperatures) than adults. Fortunately, it is rare for the source of the fever to be life-threatening, so here we will answer some common questions for parents who have a kid with a fever.*
What is considered a fever?
We define a fever as a body temperature over 100.3℉ (or 38.0℃). A fever is not inherently dangerous to your child and is, in fact, a natural response to any sort of illness (and not necessarily an infection). There are many conditions, in addition to infections, that can elicit an elevated body temperature. These include trauma or injury, inflammation, pain, even excessive clothing or being in the hot sun.
What are the common causes of a fever in a kid?
The most common cause of a fever in a child, by a landslide, is a viral illness. It can sometimes be difficult to distinguish viral from bacterial infections, but there are some very important differences between these two different categories of illness. First, viral infections are much more common than bacterial infections (the ‘common cold’, for example, is caused by a virus). There are thousands of different types of viruses that commonly cause infections, and can lead to an array of different symptoms in kids:
- isolated fever without any other symptoms
- conjunctivitis (eye redness, itching, drainage)
- earaches
- runny nose, sore throat, cough
- belly pain, vomiting, diarrhea
- rashes
- body aches, joint and muscle pain
- headache
While the majority of fevers come from a virus, which is rarely life-threatening and resolve on their own, there are a number of bacterial infections that are common in the pediatric population. Urinary tract infections are the most common type of bacterial infection in kids, but some types of pneumonia, ear infections, throat infections, and skin infections can be bacterial as well.
What can I give my child for their fever?
There are two medicines that we typically give to children for a fever: acetaminophen (Tylenol) and ibuprofen (Advil or Motrin). It is important to understand that we give these medicines to help keep the child comfortable, as fevers can often be accompanied by body aches and pains, headache, nausea or loss of appetite, uncomfortable hot or cold sensations, the list goes on. Again, the fever itself is not dangerous, and in fact, is a natural response to infection that helps the child fight infection (there is even evidence to suggest that medicines used to bring down a fever may prolong the illness duration).
The primary medicine used for fever in a child is acetaminophen (Tylenol). Pediatricians recommend acetaminophen doses of 10-15 mg/kg per dose, every 4 to 6 hours, for patients over 3 months old. (Please note that you should not exceed a total dose of 90 mg/kg in a day.) You will typically see an effect within 30 to 60 minutes, but it is important to note that 20% of children will have a persistent fever despite Tylenol administration (and this has no implications for the severity of the infection, so don’t worry if your child’s fever does not come down).
Table below to help provide clarification (and dosing based on pounds).
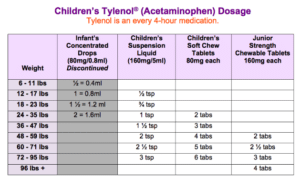
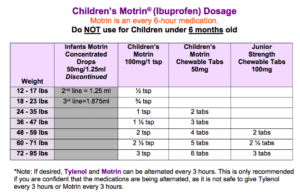
It has become an increasingly common practice to also combine this with ibuprofen (Advil or Motrin). Ibuprofen can be given at a dose of 10mg/kg, every 6 hours, for patients over 6 months old (and not to exceed 40 mg/kg per day).
When should I bring my child to an ER for a fever?
In most cases, a child with a fever does not require emergent workup or treatment, and it is safe to monitor your child’s fever and symptoms at home (or make an appointment with his or her pediatrician, if necessary). There are certain circumstances, however, where it is best not to delay evaluation. A quick call to your pediatrician’s office is helpful, and someone on staff can often help you evaluate your child’s condition over the phone. If you are unable to get in touch with a clinician, here is some guidance on when an ED visit is necessary.
If your child is UNDER 3 MONTHS old, you should proceed to the nearest ED for:
- any fever over 100.3 degrees
- excessive lethargy, or difficulty arousing the baby
- the baby is unwilling (or too sleepy) to feed
- vomiting
- rapid breathing, difficulty breathing, excessively noisy breathing
- presence of rash
If your child is 3 MONTHS TO 3 YEARS old, and their fever is accompanied by any of the additional symptoms:
- excessive lethargy or difficult to arouse
- signs of dehydration (significant decrease in urination, sunken eyes, tearless crying)
- inability to keep down any fluids
- rapid breathing, difficulty breathing, excessively noisy breathing
- fever in a non-immunized child
If your child is OVER 3 YEARS old, and their fever is accompanied by any of the additional symptoms:
- abdominal pain (children with fevers will often complain of a tummy ache, but if they seem to be in severe pain, crunched over, or unwilling to move because of the pain, this is more worrisome)
- excessive lethargy or difficult to arouse
- signs of dehydration (significant decrease in urination, sunken eyes, tearless crying)
- difficulty breathing
- stiff neck
What will they do in the ER?
If you bring your child to the ED for a fever, their doctor will determine if any tests (or treatment) are needed based on the child’s age, symptoms, immunization status, and physical exam. In most cases, all that is needed is a good history and exam, and no additional testing or treatments will need to be administered in the ED. The doctor or nurse will take time to review the medicines and supportive care measures you can continue at home to care for your child as the fever and illness run its course.
If further testing is needed, this is determined on a case-by-case basis. The testing may be as simple as a urine test or throat swab or may include a blood draw and full set of lab work, radiographic images such as a chest X-ray or abdominal CT scan, or possibly even a lumbar puncture to evaluate for meningitis. This testing helps us decide if the child needs any further treatment, such as IV fluids for dehydration, antibiotics for bacterial infection, or even hospitalization for treatment. More often, however, the testing is reassuring and indicates that no further treatment or testing is indicated.
*Please note, these recommendations are for children who are otherwise healthy without underlying medical conditions.